Polycystic Ovary Syndrome (PCOS) is a condition that affects millions of women worldwide. It is a hormonal disorder that can cause various symptoms, including irregular periods, excessive hair growth, and difficulty getting pregnant. In recent years, PCOS has become a significant topic in reproductive endocrinology, as its impact on fertility and overall reproductive health has become more apparent. In this blog post, we will discuss the role of PCOS in reproductive endocrinology and its implications for women trying to conceive.
Firstly, let’s understand what PCOS is and how it affects the reproductive system. PCOS is a condition that affects the ovaries, causing them to produce higher levels of androgens (male hormones) than usual. This hormonal imbalance can lead to irregular ovulation and menstrual cycles, as well as the development of small cysts on the ovaries. These cysts are not harmful but can contribute to the production of excess androgens, leading to further hormonal imbalances.
One of the most significant impacts of PCOS on reproductive endocrinology is its effect on ovulation. Ovulation is the process by which the ovaries release an egg each month, which can then be fertilized by sperm. In women with PCOS, ovulation may not occur regularly or at all, making it challenging to conceive. This is because the hormonal imbalances caused by PCOS disrupt the normal ovulation process. Without ovulation, there is no egg available for fertilization, and therefore pregnancy cannot occur.
Furthermore, PCOS can also affect the quality of a woman’s eggs. Studies have shown that women with PCOS have a higher number of immature eggs and a lower number of mature eggs compared to women without the condition. This can make it more difficult for women with PCOS to conceive, even if they do ovulate regularly. Additionally, the hormonal imbalances caused by PCOS can also affect the uterine lining, making it less conducive for implantation and pregnancy.
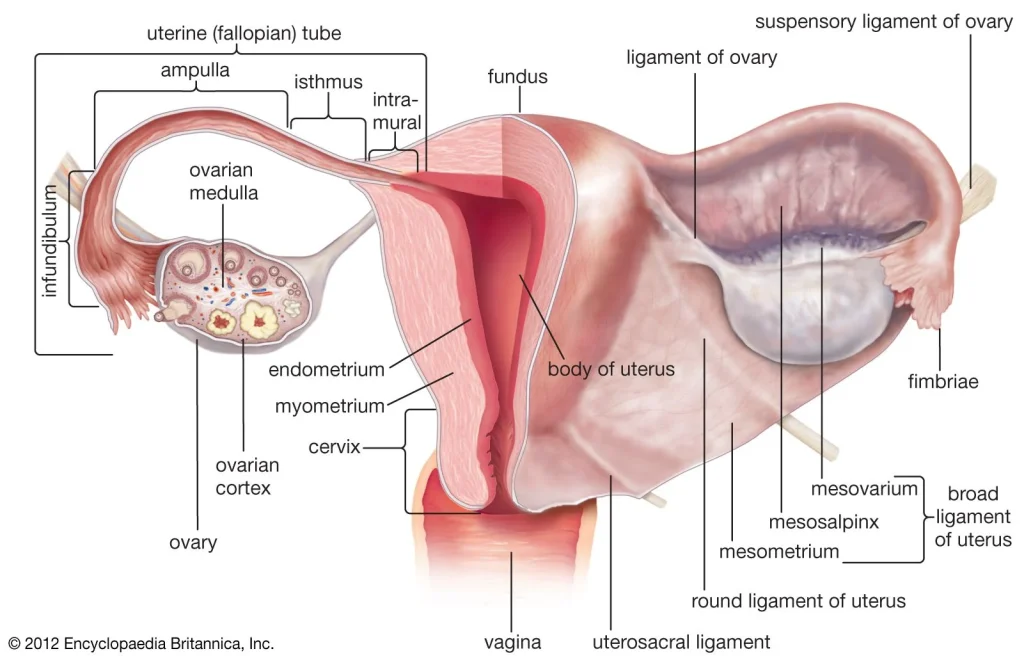
The Role of Polycystic Ovary Syndrome in Reproductive Endocrinology
Another aspect of reproductive endocrinology impacted by PCOS is insulin resistance. Insulin is a hormone that helps regulate blood sugar levels, but women with PCOS often have higher levels of insulin in their bodies. This can lead to insulin resistance, where the body’s cells do not respond adequately to insulin. Insulin resistance has been linked to an increased risk of miscarriage and gestational diabetes, both of which can affect a woman’s ability to conceive and maintain a healthy pregnancy.
The link between PCOS and reproductive endocrinology also extends to the menstrual cycle. Women with PCOS often have irregular periods or may experience long gaps between periods. This is because the hormonal imbalances caused by PCOS can disrupt the normal hormonal fluctuations that occur during the menstrual cycle. This can make it challenging to track ovulation and plan for pregnancy, as ovulation may not occur at the expected time in the cycle.
Apart from the physical impact of PCOS on reproductive endocrinology, there are also emotional and psychological effects to consider. Many women with PCOS struggle with body image issues, particularly due to the excess hair growth and weight gain often associated with the condition. This can lead to mental health issues, such as anxiety and depression, which can further affect a woman’s ability to conceive. It is essential to address these emotional and psychological aspects of PCOS to support women in their fertility journey.
So, what can be done for women with PCOS who are trying to conceive? The first step is to seek medical assistance from a reproductive endocrinologist. They can diagnose PCOS and assess its impact on a woman’s fertility and overall reproductive health. Treatment options may include lifestyle changes, such as diet and exercise, to manage insulin resistance and improve hormonal balance. Medications, such as oral contraceptives and fertility drugs, may also be prescribed to regulate ovulation and improve fertility.
In conclusion, PCOS plays a significant role in reproductive endocrinology and can have a profound impact on a woman’s fertility and overall reproductive health. It is crucial for women with PCOS to seek medical assistance and work with a reproductive endocrinologist to manage the condition and improve their chances of conceiving. With the right support and treatment, women with PCOS can overcome the challenges and achieve their dream of starting a family.